The benefits of automating your revenue management processes are clear. From reduced costs to enhanced care, happier patients to more satisfied staff, automation delivers measurable value at each stage of the revenue cycle.
While healthcare leaders understand the importance of shifting to an automated strategy, the “how” is less clear. What does it take to realize the benefits of true autonomous revenue cycle management?
Identify your level of revenue management maturity
When your organization begins to prioritize digital transformation of the revenue cycle, it can help to set a benchmark. Identifying where you are today can help clarify where you want to be tomorrow, as well as define the steps along the way.
We think of revenue management maturity in six levels.
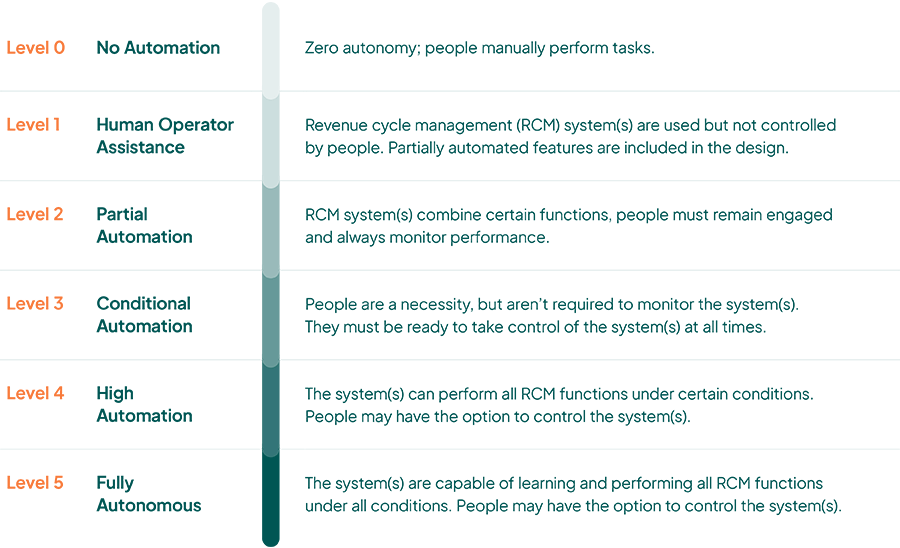
As organizations move up in level of automation, administrative costs decrease and benefits to the stakeholders increase. At Level 0, staff are too tied up with administrative tasks to focus on improving patient care. At Level 5, cutting-edge AI and ML technologies are learning and performing all RCM functions, allowing healthcare organizations to focus on what matters most—serving their patient populations and establishing a healthy bottom line.
Most health systems’ revenue cycle management processes are operating at Level 1 in terms of automation maturity – and that’s okay. The key factor is that the organization and leadership see the vision and are dedicated to realizing it.
Five steps to advance your autonomous revenue cycle strategy
What does it take to climb the ladder to move toward a level-five approach to RCM? Working with our customers, we have defined the essential building blocks of an automated approach.
Advancing autonomous RCM requires a deep commitment to breaking down data silos, retraining colleagues, and improving workflow integration across interconnected systems such as financial clearance, charge capture, coding, claims, payer adjudication, denials management and collections. The entire revenue management process must be anchored in a unified data environment to flow smoothly and continuously. While this may seem like a hefty lift, it will create long-term efficiencies that will benefit everyone.
To support the shift to autonomous revenue management, healthcare leaders need to say “Yes” to these 5 simple steps:
- Start small.
Deal with low-hanging fruit first. Begin with data-rich tasks that are manual, repetitive and easily automated. - Invest in technology.
Analytics, RPA and AI/ML are the building blocks of an autonomous revenue cycle. These tools will allow you to build powerful algorithms and data interfaces that will intelligently automate all pieces of the revenue cycle. Investing in these emerging technologies and deploying them throughout the continuum of your revenue cycle will optimize your processes, increase efficiencies and improve your bottom line. - Invest in people.
Building the framework for an autonomous revenue cycle requires specialized data science expertise in AI and ML. The best and brightest will need to be employed to build necessary algorithms. In addition, all employees who touch any portion of the revenue cycle will need ongoing training, education and upskilling, as well as structured career paths in order to keep them engaged in the process. - Break down data silos.
Harnessing the vast amount of available revenue cycle data is key. Typically, systems focus on the data needed to be acted upon (the claim, encounter, etc.), but fail to gather data on how users interact with the data and systems. Once an optimal process of completing the work is identified, the task can then be automated. - Unite in a common goal.
Each player in the revenue cycle has its own strengths. When they join forces and look at ways to build trusted systems that automatically adjudicate payments, they can collectively help achieve the holistic view needed to achieve an autonomous revenue cycle.
FinThrive: Your trusted partner for autonomous revenue cycle management
FinThrive is proud to play a critical role in advancing our customers’ automated revenue management strategies. We pride ourselves on providing the most complete end-to-end revenue management platform in healthcare. With decades of experience, transformative innovation and thousands of happy customers, we’ve got the technology, expertise and scale to deliver a frictionless revenue experience.
Read the full guide on how end-to-end autonomous revenue cycle management from FinThrive helps organizations confidently move toward profitability. Or if you are ready to speak to us now, contact FinThrive.







